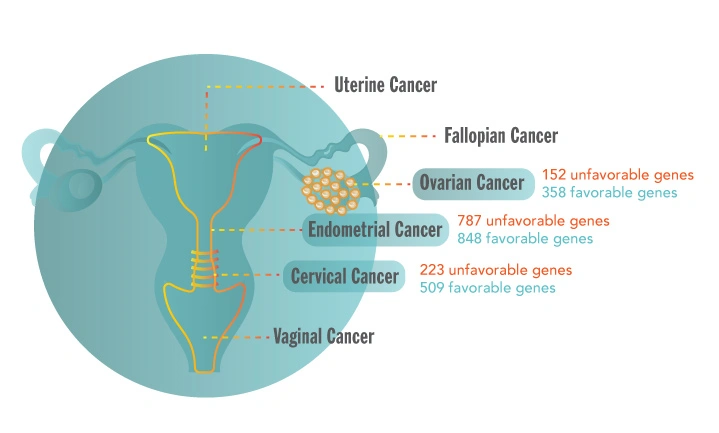
Gynecological cancers—including ovarian, endometrial, and cervical tumors—are marked by remarkable biological diversity. Their molecular signatures often predict tumor progression, therapy response, and recurrence risk.
Prognostic biomarkers serve as critical molecular indicators that reveal this underlying biology, offering insights far beyond traditional histopathology.
1. Why Biomarkers Are Essential in Modern Pathology
In diagnostic and prognostic pathology, biomarkers act as molecular signposts that define tumor behavior with precision. They enable pathologists to:
- Assess proliferation using markers like Ki-67
- Identify genomic instability, for example through abnormal p53 or p16 expression
- Detect features associated with invasion and metastasis, such as L1CAM or MUC16/CA125
- Characterize hormone signaling, tumor differentiation, and microenvironment interactions
Integrating these protein-level markers with tissue morphology provides a more nuanced understanding of tumor aggressiveness and patient risk.
2. Driving Basic Research and Translational Discovery
Prognostic biomarkers are active indicators of tumor biology rather than passive descriptors. Their expression reflects dysregulated pathways—such as PI3K/AKT signaling, p53-dependent DNA repair, or HPV-mediated cell-cycle disruption—that drive proliferation, invasion, and therapy resistance. Many also reveal how tumors manipulate the microenvironment and evade immune surveillance through EMT, extracellular matrix remodeling, or checkpoint signaling.
By linking these molecular alterations to clinically relevant outcomes, biomarkers guide the identification of subtype-specific vulnerabilities, inform preclinical models, and accelerate translational research toward targeted therapies and more predictive disease models.
3. Examples of Powerful Biomarkers Across Gynecological Tumor Types
Endometrial Cancer
- L1CAM: Strongly associated with recurrence and poor survival, especially in high-grade or non-endometrioid tumors, reflecting increased invasiveness.
- p53 (TP53): Aberrant expression signals genomic instability and aggressive disease.
- ER and PR (ESR1, PGR): Hormone receptor status informs prognosis and therapeutic planning.
Cervical Cancer
- p16^INK4a: A hallmark of high-risk HPV-driven transformation, indicating lesion progression and proliferative activity.
- Ki-67 (MKI67): Quantifies proliferation, helping identify high-risk lesions.
- PD-L1 (CD274): An immune checkpoint marker increasingly studied for prognostic and therapeutic relevance.
Ovarian Cancer
- MUC16 (CA-125): Reflects tumor burden and dissemination, useful for monitoring progression and recurrence.
- HE4 (WFDC2): Associated with aggressive serous and endometrioid ovarian cancers, predictive of recurrence.
- E-cadherin (CDH1): Loss of adhesion correlates with invasiveness and metastatic potential.
4. Combining Biomarkers for Greater Prognostic Precision
Single biomarkers provide valuable insights, but integrated biomarker panels offer a more powerful approach to stratify patients and guide therapy. By combining markers of proliferation, genomic instability, hormone signaling, and immune evasion, researchers and clinicians can:
- Identify high-risk subgroups more accurately than with individual markers
- Predict treatment response to targeted therapies or immunomodulators
- Develop multi-dimensional models linking molecular profiles to clinical outcomes
- Reveal synergistic interactions between pathways that drive tumor progression
Examples:
Endometrial Cancer : pairing L1CAM and p53 in endometrial cancer highlights aggressive non-endometrioid subtypes,
Ovarian cancer: combining HE4 and MUC16 in ovarian cancer improves prognostic discrimination for serous tumors.
Cervical cancer: In cervical cancer, p16 together with Ki-67 allows refined assessment of lesion grade and proliferation.
These multi-marker approaches are increasingly essential in both research and translational settings, providing a roadmap for precision oncology.
5. Atlas Antibodies: Advancing Gynecological Cancer Research with High-Specificity Antibodies
Our high-quality, application-validated antibodies are essential for studying prognostic biomarkers in tissues and experimental models.
They enable:
- Robust immunohistochemistry to visualize protein expression in patient samples
- Accurate quantification in cell lines, organoids, and tissue models
- Reproducible biomarker validation for translational and preclinical studies
- Identification of novel therapeutic targets and molecular mechanisms
Discover our portfolio of validated antibodies for gynecological cancers and power your next experiment with precision and confidence.
Prognostic Markers in Gynecological Cancers
